Stress vs. Burnout: Brain Differences
Stress and burnout both impact the brain, but in very different ways:
- Stress is a short-term response to pressure, activating the brain's survival systems. It temporarily disrupts areas like the prefrontal cortex (decision-making) and enhances the amygdala (threat detection). Once the stressor is gone, the brain typically recovers within hours or days.
- Burnout, on the other hand, results from prolonged stress and causes long-term damage. Key brain regions, like the prefrontal cortex and hippocampus (memory and learning), shrink, while the amygdala becomes hypersensitive. These changes lead to persistent cognitive issues, emotional exhaustion, and impaired decision-making.
Understanding the neurological differences between stress and burnout can help leaders recognise early warning signs and take action to prevent lasting damage. Leaders should prioritise recovery strategies, such as quality sleep, regular exercise, and reducing mental strain, to maintain cognitive health and long-term effectiveness.
The Brain-Damaging Effects of Chronic Stress and Burnout | Rochelle Walsh
sbb-itb-ce676ec
How Stress Affects the Brain: Short-Term Response
Understanding the brain's immediate response to stress reveals how it manages short-term challenges, highlighting the contrast with the long-term effects seen in burnout.
Stress sets off an adaptive chain reaction aimed at quick mobilisation and recovery. When the brain perceives a threat - whether it's a tight deadline or an unexpected crisis - it activates a survival system. Central to this is the hypothalamic-pituitary-adrenal (HPA) axis. The hypothalamus signals the pituitary gland, which in turn prompts the adrenal glands to release cortisol and adrenaline into the bloodstream. Blood flow is redirected from non-essential functions, such as digestion, towards the muscles, while glucose is swiftly made available to supply energy. When the stressor is resolved, this response helps build resilience, showcasing its adaptive nature. Below, we explore the key neurological processes driving this stress response.
The HPA Axis in Stress
The HPA axis responds within seconds of detecting a threat, reallocating resources to ensure survival. In a healthy system, once the danger passes, the prefrontal cortex and hippocampus signal the HPA axis to deactivate, allowing cortisol levels to return to normal.
Effects on the Prefrontal Cortex
Acute stress temporarily disrupts the prefrontal cortex, the brain's "command centre." A surge of norepinephrine and dopamine weakens synaptic connections in this region. This neurochemical shift hands control over to more instinctive brain areas, such as the hypothalamus and basal ganglia, which are better suited to rapid, survival-focused decisions. This change often results in a temporary decline in cognitive abilities, including memory, focus, and impulse control. Typically, cortisol levels peak and begin to subside within 20 to 60 minutes, allowing the prefrontal cortex to recover if the stressor is resolved.
"The prefrontal cortex takes a backseat. The amygdala takes the wheel. You stop thinking carefully and start reacting fast." – AJ Keller, CEO, Neurosity
Amygdala and Threat Response
As the prefrontal cortex becomes less active, the amygdala - the brain's threat detection hub - takes on a heightened role. It alerts the nervous system to prepare for immediate action and enhances the storage of fear-related memories, aiding future threat recognition. This shift enables rapid responses, such as freezing, fighting, or fleeing, rather than slower, deliberate reasoning. Professor Amy Arnsten of Yale University notes that freezing, for example, can reduce detection by predators and improve survival chances in immediate danger. For leaders, this mechanism might translate into instinctive reactions under pressure - effective in the short term but unsustainable if the stress persists.
Burnout: Long-Term Brain Dysfunction
Stress, in small doses, can help the brain adapt and respond to challenges. However, when stress becomes chronic and unchecked, it can result in lasting changes to the brain. Burnout isn’t just prolonged stress - it represents a breakdown in the brain’s ability to balance threat and reward. As the Association for Psychological Science notes, "Burnout is not just a state of mind, but a condition that leaves its mark on the brain as well as the body". Unlike the temporary effects of acute stress, burnout causes structural alterations in the brain, leading to long-term dysfunction. The systems designed to protect the brain begin to cause harm, resulting in significant neurological disruptions.
HPA Axis Overactivation and Allostatic Load
The hypothalamic-pituitary-adrenal (HPA) axis, which regulates the body’s stress response, becomes hyperactive during acute stress, releasing cortisol to help manage immediate challenges. However, under chronic stress, this system can become overwhelmed and eventually dysfunctional. Initially, cortisol levels remain persistently high, flooding the brain with stress hormones. Over time, the system may collapse into a state known as hypocortisolism, where cortisol production becomes insufficient. This creates a paradoxical state often described as "wired but tired", where the stress response system fails to shut down properly. The result is low-grade inflammation and widespread exhaustion. Research highlights the severe physical toll of burnout: employees in the top 20% of burnout scales face a 79% higher risk of coronary heart disease, while executives are 2.5 times more likely to experience heart attacks.
Prefrontal Cortex Damage
Chronic stress doesn’t just disrupt the prefrontal cortex temporarily - it causes structural thinning of its grey matter. This region, crucial for decision-making and emotional regulation, can lose up to 20% of its volume under prolonged stress. Professor Amy Arnsten from Yale School of Medicine explains: "One of the most striking (effects) is thinning of the grey matter of an area of the brain called the prefrontal cortex... It allows us to do complex decision-making and to be able to have thoughtful, abstract reasoning rather than concrete or habitual responses". For leaders, this damage manifests as persistent brain fog, indecision, and difficulty with strategic thinking. The prefrontal cortex’s diminished capacity also weakens emotional regulation, making it harder to manage impulses or maintain focus.
Amygdala Oversensitivity
Burnout also leaves a mark on the amygdala, the brain’s emotional processing centre. In individuals with burnout, the amygdala becomes not only more sensitive but also enlarged. A 2014 study led by Armita Golkar at the Karolinska Institutet compared 40 individuals with burnout to 70 healthy controls using fMRI scans and startle-response tests. The results showed significantly enlarged amygdalae in the burnout group, along with reduced connectivity between the amygdala and the medial prefrontal cortex. This heightened sensitivity explains why people with burnout often struggle to regulate negative emotions. The amygdala’s alarm system remains stuck in an "on" position, causing minor setbacks to feel like major threats. This contributes to emotional exhaustion, heightened anxiety, and a sense of detachment - even in otherwise safe environments. For leaders operating in high-pressure roles, these neurological changes highlight the importance of addressing burnout before it undermines their decision-making and emotional resilience.
Stress vs. Burnout: Brain Differences Compared
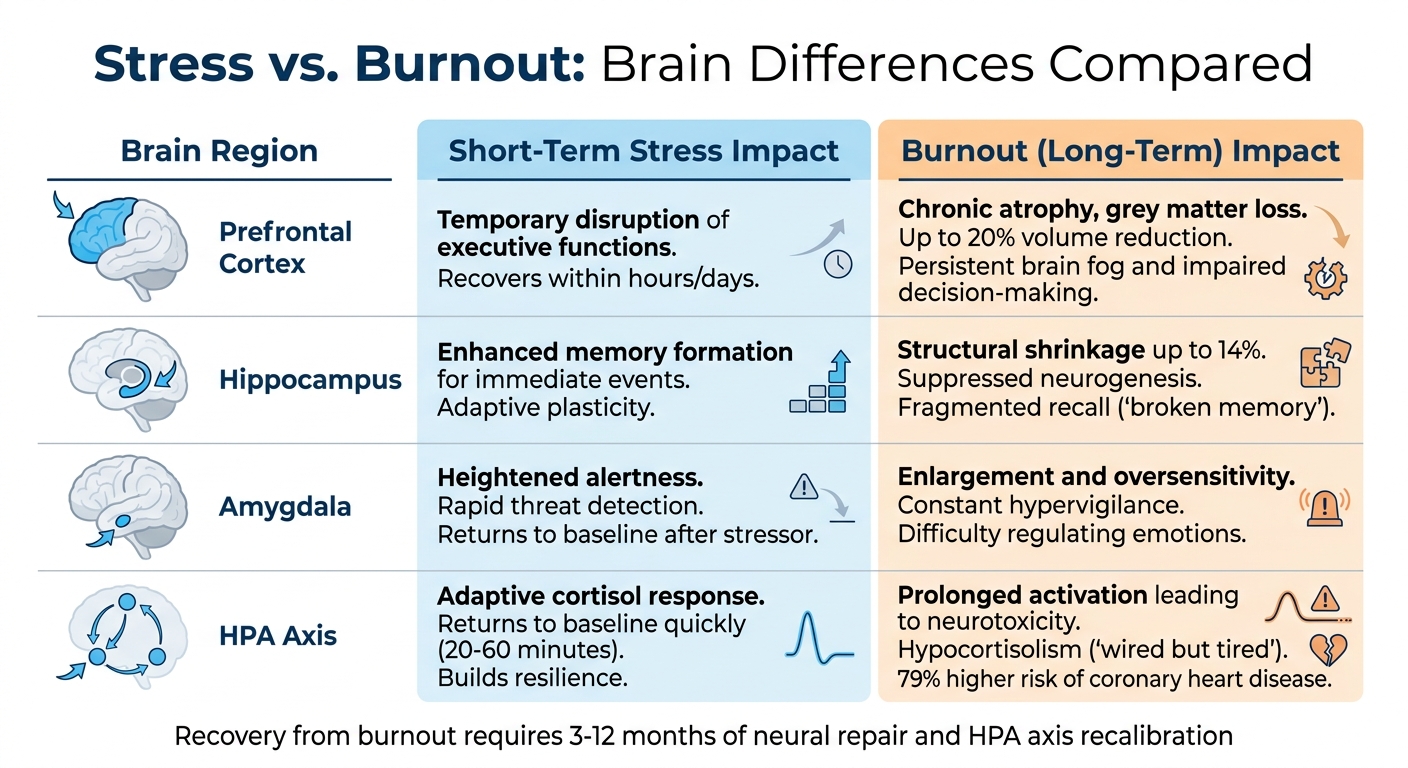
Stress vs Burnout Brain Effects Comparison Chart
Acute stress and burnout affect the brain in fundamentally different ways. While acute stress causes temporary disruptions, burnout leads to lasting structural changes that require deliberate intervention. To understand these distinctions, it’s essential to explore how these conditions uniquely impact key brain regions.
Prefrontal Cortex: Short-Term Disruption vs. Long-Term Damage
The prefrontal cortex, often referred to as the brain's "executive control centre", temporarily shifts into a lower gear during acute stress. This allows survival instincts to take precedence. Once the stressor is removed, the prefrontal cortex typically resumes full functionality within hours or days.
Burnout, however, causes more severe and lasting effects. Chronic stress leads to dendritic atrophy, reduced grey matter density, and cortical thinning in this region. These changes manifest as persistent cognitive impairments, including brain fog, poor decision-making, and reduced impulse control. Essentially, the brain's "CEO" becomes consistently less effective.
| Brain Region | Short-Term Stress Impact | Burnout (Long-Term) Impact |
|---|---|---|
| Prefrontal Cortex | Temporary disruption of executive functions | Chronic atrophy, grey matter loss, and impaired cognition |
| Hippocampus | Enhanced memory formation for immediate events | Structural shrinkage, suppressed neurogenesis, and memory loss |
| Amygdala | Heightened alertness and rapid threat detection | Enlargement, oversensitivity, and constant hypervigilance |
| HPA Axis | Adaptive cortisol response that returns to baseline quickly | Prolonged activation, leading to neurotoxicity and imbalance |
Hippocampus: Adaptive Plasticity vs. Structural Shrinkage
Acute stress can temporarily benefit the hippocampus, enhancing memory to help individuals remember critical details about a threat. This evolutionary adaptation is designed to improve survival by making it easier to recognise similar dangers in the future.
In contrast, burnout causes significant structural damage to the hippocampus. Studies have shown that individuals with prolonged cortisol exposure can experience hippocampal shrinkage of up to 14%, along with noticeable memory deficits. Chronic stress also suppresses neurogenesis - the process of creating new neurons - resulting in fragmented recall often described as "broken memory". This damage undermines the hippocampus's ability to differentiate genuine threats from false alarms, exacerbating feelings of overwhelm.
The hippocampus’s deterioration under burnout also aligns with changes observed in the amygdala, further highlighting the interconnectedness of these brain regions.
Amygdala: Temporary Alertness vs. Lasting Oversensitivity
In the short term, stress activates the amygdala, sharpening alertness and improving the ability to detect threats. Once the immediate danger has passed, the amygdala typically calms down, returning to its baseline state.
Burnout disrupts this balance. Chronic stress enlarges the amygdala, increasing its sensitivity and keeping the brain in a constant state of hypervigilance. This overactive "alert mode" can lead to heightened anxiety and difficulty regulating emotional responses. These changes underscore the importance of recognising how prolonged stress impacts the brain and why leaders should remain vigilant about these shifts to adjust their approaches effectively.
What This Means for High-Stakes Leaders
Understanding the distinction between stress and burnout’s neurological effects can help leaders protect their mental and emotional well-being. This knowledge isn’t just theoretical - it reshapes how leaders should evaluate their own performance and that of their teams. Unlike physical fatigue, where muscle exhaustion provides an obvious signal, cognitive depletion often goes unnoticed. Leaders may unknowingly push through, delivering subpar results as their prefrontal cortex becomes overwhelmed, ultimately risking long-term neurological damage.
Recognising Early Warning Signs
Burnout often begins with subtle neurochemical shifts rather than obvious behavioural changes. A decline in dopamine, norepinephrine, and acetylcholine levels can lead to reduced motivation, difficulty concentrating, and impaired memory. Leaders who previously thrived on tackling complex challenges may find themselves emotionally detached from their work.
One key indicator is compensatory effort - when leaders maintain their output by exerting extra mental energy. This hidden strain can go undetected until the brain’s ability to compensate is depleted. Another red flag is disrupted cortisol rhythms, which can create a “tired but wired” state where cortisol levels remain elevated at night. This interferes with the brain’s ability to repair itself during sleep. Persistent insomnia, especially when paired with exhaustion, should be seen as a warning sign rather than a simple case of poor sleep habits.
To address these risks, leaders might consider objective monitoring tools, such as regular neurological assessments, alongside self-awareness. Early detection is essential for managing stress and preventing burnout.
Emotional Discipline in Leadership
Emotional discipline serves as both a preventive tool and a recovery method for the brain under stress. By managing emotional responses, leaders can reduce overactivation of the amygdala, preventing the structural and functional changes associated with burnout. Developing this skill involves creating neural pathways that support measured, thoughtful reactions.
Organisations like House of Birch offer tailored advisory services to help leaders strengthen emotional discipline. Their programmes focus on protecting the prefrontal cortex from chronic overuse while maintaining effective decision-making under pressure. Emotional discipline, when approached as a trainable skill, benefits from consistent practice and expert guidance.
Leaders should also adopt a “neurochemical budgeting” approach, treating resources like dopamine and norepinephrine as finite. To maximise these reserves, schedule cognitively demanding tasks during the first 90 minutes of the day, when neurochemical levels are highest. Additionally, minimising context-switching is essential, as it takes approximately 23 minutes to regain focus after an interruption. These strategies not only prevent burnout but also support recovery and resilience over time.
Recovery and Resilience Techniques
Once early signs of burnout are identified, recovery practices become critical. True recovery requires 3 to 12 months of neural repair and recalibration of the hypothalamic-pituitary-adrenal (HPA) axis; short breaks are insufficient to reset cortisol levels. Leaders must prioritise restorative sleep - 7 to 9 hours per night - to allow the brain’s glymphatic system to clear metabolic waste. It’s worth noting that only 1% of people possess the DEC2 genetic variant enabling them to function well on less than 6 hours of sleep.
Moderate aerobic exercise, such as 30 to 60 minutes of activity three to five times a week, can stimulate the release of Brain-Derived Neurotrophic Factor (BDNF). This supports hippocampal neurogenesis, helping reverse structural damage in the brain. Similarly, spending at least 20 minutes daily in natural environments reduces amygdala activity and improves attention capacity. These aren’t optional wellness activities - they are essential for leaders under sustained pressure.
Leaders can also apply the “5% Rule”: focus on the first 5% of a project, setting the strategic direction, and then delegate the rest. This preserves cognitive resources while enhancing team performance. Anil K. Singhal’s The 5% Rule of Leadership, highly rated on Amazon, explores how this principle can mitigate burnout and prevent team inefficiencies.
Lastly, chronic stress associated with burnout can lead to astrocytic phagocytosis, where brain maintenance cells consume healthy synapses, accelerating neural decline. This underscores why recovery from burnout is a long-term process requiring sustained intervention, as structural changes in the brain’s prefrontal cortex, hippocampus, and amygdala demand time and deliberate effort to repair.
Conclusion
The neurological distinctions between stress and burnout highlight critical differences in brain function, each requiring tailored responses. While acute stress temporarily disrupts brain activity, burnout causes enduring structural damage, necessitating a prolonged recovery process. This distinction is not just theoretical - it has profound implications for how leaders approach their own cognitive health and manage their teams.
Research shows that prolonged stress, marked by excessive neural resource allocation and increased P3 amplitude, can overwhelm the brain's compensatory systems. This has measurable organisational consequences, including a 42% decline in team engagement and a 31% drop in productivity.
"We need to start looking at occupational burnout as a problem with the brain." - Kaisa Hartikainen, Clinical Neurologist and Brain Scientist, University of Tampere
Organisations like House of Birch offer leadership advisory services that integrate neuroscience insights. Their programmes focus on emotional regulation, decision-making under pressure, and strategic thinking to help leaders preserve prefrontal cortex function and strengthen the neural pathways essential for sound decision-making.
The evidence underscores the importance of early intervention. Acting early allows leaders to harness the brain's neuroplasticity to reverse harmful changes. In contrast, delayed action - once structural damage and cortisol dysregulation have set in - makes recovery far more challenging. Leaders who understand these neurological dynamics can better balance pushing forward with implementing recovery strategies, ultimately protecting their cognitive resilience and long-term effectiveness.
FAQs
How can I tell if I’m stressed or burnt out?
Stress tends to be a short-term reaction to particular challenges and often subsides with adequate rest. Burnout, on the other hand, is a long-term condition driven by sustained stress. It manifests as emotional exhaustion, a sense of detachment, and a noticeable drop in productivity. Beyond these symptoms, burnout also impacts brain function, disrupting memory, decision-making abilities, and emotional stability. If taking time to rest doesn’t alleviate the symptoms and they persist, it’s likely a sign of burnout. Understanding this distinction is crucial for identifying effective recovery methods.
Can burnout brain changes be reversed?
Burnout can cause noticeable changes in the brain, but these effects aren’t permanent. With consistent and targeted interventions, the brain can gradually restore and rewire itself. This recovery process, however, isn’t immediate - it demands time, persistence, and regular attention to mental health and overall well-being. Small, steady efforts over time can make a meaningful difference.
What are the earliest warning signs leaders should watch for?
Leaders need to remain vigilant for signs such as emotional exhaustion, cynicism, irritability, dwindling motivation, and challenges in decision-making. These indicators often point to early neurobiological changes associated with burnout, including damage to the hippocampus and heightened activity in the amygdala due to extended periods of stress. Recognising these symptoms promptly can play a crucial role in mitigating further harm to both mental and physical well-being.
